NHS England’s annual report and accounts say they have delivered on objective four of the government’s mandate to the NHS
Objective 4: Embed a population health management approach within local systems, stepping up action to prevent ill health and tackle health disparities
In meeting the requirement, NHS England reports The NHS Digital Weight Management Programme has been successfully operational since 2021 and yielded 240,000 referrals by March 2023.
TTE has concerns that, as a funder, NHS England is commissioning itself to deliver on population health management projects. Usually, that would be seen as a direct conflict, as one might tend towards pet projects that might not be the best use of funds. Therefore, TTE looked into whether the NHS Digital Weight Management Programme is the best use of funds to deliver population health.
On the NHS England website, the NHS Digital Weight Management Programme supports adults living with obesity who also have a diagnosis of diabetes, hypertension, or both to manage their weight and improve their health. It is a 12-week online behavioural and lifestyle programme that people can access via a smartphone or computer with internet access.
The program has hidden costs. First, you have to speak to your GP or a local pharmacist to be referred to the program. The irony, though, is that the website says, “Please note that GP and pharmacy teams may be very busy at this time.”
Once enrolled, you’ll receive a text message to sign up, and your chosen weight management plan provider will contact you.
A total of six providers are listed.
Second Nature: includes a 12-week program, ongoing access, and support from a registered dietitian or nutritionist.
Slimming World: A provider of the NHS Digital Weight Management Programme.
Liva Healthcare: A provider of the NHS Digital Weight Management Programme.
Oviva: A provider of the NHS Digital Weight Management Programme.
MoreLife: A provider of the NHS Digital Weight Management Programme.
Xyla Health and Wellbeing: A NHS Digital Weight Management Programme provider.
It’s hard to know the actual costs of these programs; Second Nature reports the weight loss programme cost and ongoing support as £28 per month. If you throw in the GP appointments and hidden fees, we estimate costs could be roughly £150 per person for a twelve-week course. In the NHS England report, there were 240,000 referrals by March 2023, at an estimated cost of £36 million.
But what does NHS England get for their money?
An evaluation was highlighted as a success: The study reported that completers lost 3.9kg or 8.6 lbs over 12 weeks. Of the 31,718 people who started the initiative, including those who did not complete it, the average weight loss was still 2.2kg or 4.85 lbs.
A comparison of the effectiveness of each intervention suggested that the addition of personal coaching is positively associated with more engagement, completion, and costs.
All sounds impressive; however, let's think about the population effect.
Older people, people with disabilities, and lower-income groups are often excluded from such interventions. Currently, 22% of the population does not have the digital skills needed for everyday life, and nearly half of UK families are excluded from modern digital society. So, TTE estimates that about a third of people won't have the technology or know how to access the scheme.
The study reported that 63,937 people were referred to the scheme in its first year, and 50% accepted the offer and enrolled in the service; 14,268, less than half who took it up, completed the programme from April 2021 to March 2022.
We've converted these numbers to see what happens in a population of 1,000. By the end of 12 weeks, the intervention applies to only 156 people, and we also have no idea of what happens to these people beyond 12 weeks.
In 2013, the program Men Who Made Us Thin asked TTE about the evidence regarding whether Weight Watcher programs contribute to weight loss as a public health intervention. Like the apps, we found they don’t apply to most folks. Losing weight isn’t that difficult; keeping it off is the problem.
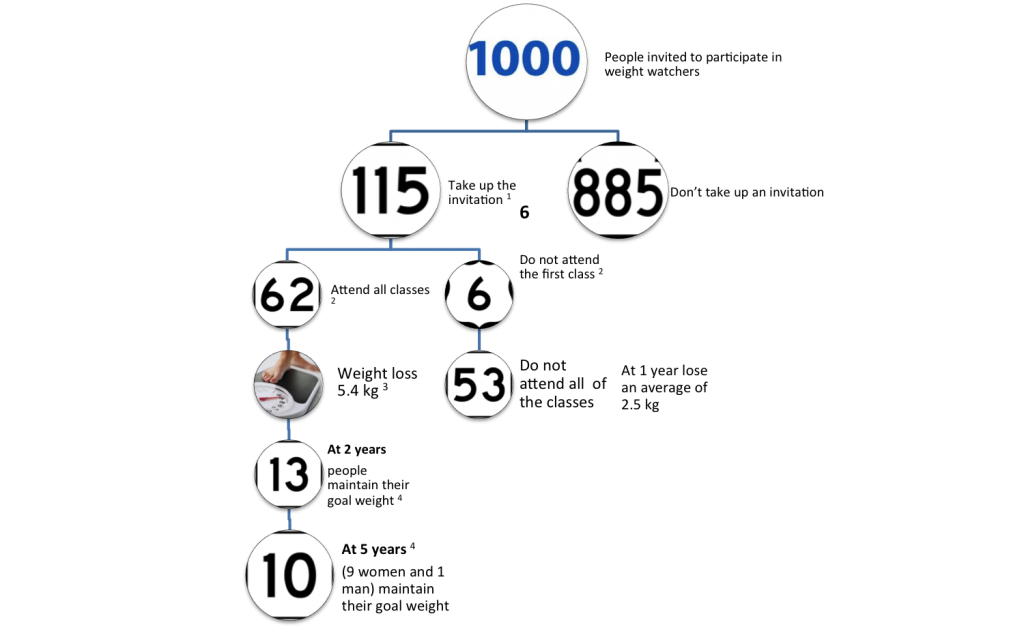
How many people out of 1000 will gain their goal weight?
NHS England provides a program that is not population-based, remains poorly evaluated, and lacks evaluation of the medium to long-term effects, the actual costs, and the genuine impact on healthcare.
The paper states, “The uncontrolled nature of this analysis means that external confounders cannot be excluded, and there may have been other factors influencing weight change.”
But despite all this, we expect to see more attempts to increase the app's use as the population-based answer to weight loss.
Recommendation
Prevent funders from commissioning themselves to implement population health programs and ensure any interventions are robustly evaluated with controlled trials in the population of interest with the essential clinical endpoints.
Potential savings to the NHS - hundreds of millions
This post was written by two old geezers who could do with losing a little weight.
References for the numbers are
Jolly et al. (BMJ): the response rate to the invitation was 11.5%
Ahern et al. (BMC Public Health): 54% of courses were completed
Ahern et al. (BMC Public Health): median weight change was 5.4kg in those that completed the course
Lowe MR (BJN) The percentage of participants who remained below their goal weight at 2 and 5 years was 20.5% and 16.2% respectively






The language alone made me shudder: "adults living with obesity" - what the fluffing fluff does that even mean? Is it now politically incorrect to say 'obese adults'? I know we mustn't 'body-shame' or, the horror, 'fat shame', but now even 'obese' must be veiled in non-hurting language?
As for the programmes themselves: the 'success' is astounding! People seem to lose as much weight per week as having drunk or not drunk a glass of water before weighing. But certainly, the 'providers' of all those programmes will become fat, or rather: their wallets will, thanks to NHS funding.
No wonder the other hand of the NHS is pushing that Zum Zum water: far more successful for shedding unwanted fat.
Oh btw - I'm 'living with old age' - do I get a piece of chocolate as reward or would that be unhealthy?
Since these strategies are based on on Calorie reduction, it is no surprise that the results are so disappointing.
In 2017, I wrote this in my blog:
The big problem with reducing calories is that it is essentially semi-starvation, which is invariably accompanied by hunger. As long ago as 1959, Albert Stunkard and Mavis McLaren-Hume reviewed the available studies (2). At the outset they stated that weight-reduction programmes are based on the assumptions that they are effective and that they are harmless. However they concluded that:
“The results of treatment for obesity are remarkably similar and remarkably poor”
They reported that only 25% of the subjects had lost as much as 8kg on their low calorie diets, while only 5% successfully lost 16kg. This was in line with his Stunkard’s experience as a physician working with 100 obese patients that were prescribed “balanced” diets of 800-1500 calories per day. He found that only 12% lost 8kg and one patient managed to lose 16kg. Even more significantly, two years after the end of the treatment only two patients had maintained their weight loss.
Those experts in the field persist in advocating calorie reduction despite the fact that there is a lack of evidence that the approach is successfully. At the same time the cases of failure continue to pile up. In the “Handbook of Obesity” by three of the leading authorities, George Bray, Claude Bouchard and Philip James it is stated that:
“dietary therapy remains the cornerstone of treatment and the reduction of energy intake continues to be the basis of successful weight reduction programs.”
However they go to accept that the results of such calorie-restricted diets:
“are known to be poor and not long-lasting.”(3).
https://vernerwheelock.com/284-obsessed-with-calories/