Lord Darzi’s independent investigation says the NHS is in critical condition. However, all is not lost, as he has a treatment plan.
The report states that the NHS is struggling after the pandemic and falling short of targets for cancer, A&E and hospital treatments, contributing to poor survival rates for cancer and heart disease.
Waiting times have "ballooned", and there's been a surge in waiting for mental health services. 2.8 million people are unable to work because of poor health.
We think Lord Darzi has been asleep for the past decade as he’s only just realised that there’s a problem with the health service and a significant problem with “the state of the nation’s health."
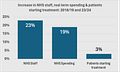
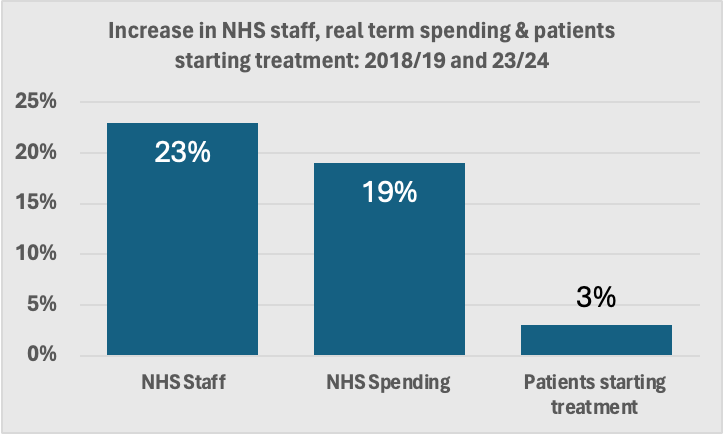
He says the austerity of the 2010s weakened the health service, yet funding has increased considerably in recent years, but productivity has decreased.
For example, the number of deliveries per midwife yearly has fallen from 34.7 in 2007 to 25.8 in 2022. Yet the solution is more money is needed - there will be a gap in funding of £27bn between health demand and funding per year by 2029/30.
The Health Secretary, Wes Streeting, told the Today programme that his focus will be improving productivity and reducing demand for the NHS. The costs could "dwarf" other areas of government spending, he said and "we'll end up with an NHS with a country attached". He added, "We've got to make sure every penny that goes in [to the NHS] is well spent,"
With an increasing ageing population and more multimorbidity than ever, restricting care will be the only way to reduce demand. The NHS remains an organisation that doesn’t know or want to embrace demand. Streeting thinks that he’ll be able to fix the problem under his tenure.
He’ll be “going hell for leather” to enact the changes that see three “big shifts” from hospital to community care, from analogue to digital and from treating sickness to preventing it.
The prevention mantra is a familiar line for a Health Secretary to trot out. Even Matt Hancock was in on the act. Hancock said: “It’s why, when I became Health Secretary, I made it one of my big three priorities alongside advancing health technology and doing much more to support our amazing health and social care workforce.” It sounds like Darzii and Streeting have been taking their advice from Hancock.
In 2009, Andy Burnham made prevention a mission for the NHS. He told the party conference that “In the next decade, our mission must be to take it from good to great, more preventative and people-centred, keeping people well and out of the hospital, empowering them to choose what they know is best for them and where they want to be treated.”
The investigation reports that spending on NHS health checks “has dropped by £15 million; participation rates in the programme have fallen by 20 percent.” Thus, the answer to all these woes will be more health checks despite evidence that they don’t work.
The second pledge that will apparently transform the NHS is “Going digital.”
In the Spring Budget of 2024, the UK government (the Tory party) announced £3.4 billion in funding for NHS digital transformation over three years, starting in April 2025. So, with this pledge in place, it remains to be seen how much extra will be allocated to the wonder treatment that is digital transformation.
Systematic reviews report moderate evidence that digital health technologies positively affect healthcare workers’ performance, mental health, management, delivery and access to care. However, most early wins, such as electronic patient records, have been rolled out, and any further investment will see diminishing returns.
Streeting also said, "As a proportion of the NHS budget, we want to shift the balance in favour of neighbourhood services."
Less money for hospitals, then. Yet, in 2023, the NHS Confederation reported, “The NHS capital budgets must nearly double to ensure crumbling buildings and infrastructure are fit for 21st-century patient care.”
“Waiting list will be millions slower than they are today,” said Streeting. Taking aside the lack of specifics, he forgets to mention the damaging effects of the lockdown and shutting down the NHS during the pandemic. The waiting lists will improve, as they can’t get any worse. However, as one part of the NHS becomes the priority, another part will suffer.
Adding gains will not result from removing unnecessary bureaucracy from NHS funding without a ruthless agenda to route out low-value care.
The Darzi report was assembled in two months. As a Lord who sat in the Labour Party until 2019, we find it unclear what part of this report is independent.
Darzi has been integral to plans to affect the NHS. In 2006, he developed a strategy to meet Londoners' health needs. In 2008, he was part of the "NHS Next Stage Review," and now leads the National Health Service’s Accelerated Access Collaborative. The answer to the NHS seems to roll out the cronies that have failed in the past.
In the TTE office, we have a straightforward rule: any simple solution to a complex problem will be wrong.
So, what does the future hold reading between the lines of the Darzi report?
It looks as if big pharma is investing heavily in big data and AI. For example, Astra Zeneca has launched a new tool called Milton, which Sky reported on in Zum Zum time:
MILTON fits in with the Darzi vision of switching from treatment to prevention. The only problem is that prevention will be achieved by identifying thousands of conditions and finding a home for “novel medicines”. Take a look:
TTE considers the focus needs to turn to preventing overdiagnosis and overtreatment, using non-evidence-based interventions, and working out what works and what doesn’t while allowing clinicians to be freed up to get on with the job of patient care.
If there is a massive problem with cancer care, then more AI won’t cut it. Reducing Cancer diagnostic time to treatment waits to one week would be a priority that most would support and is backed up by the evidence. If heart disease increases, then the golden hour targets for treatment must be met - early treatment saves lives.
The bottom line from the two old geezers is to make better use of what you already have and not chase past failures. At some point, those in power might realise they can only solve the problem from the bottom up by consulting with the people on the ground.
Republishing and reviving old policies, such as prevention, which has been the focus of previous health secretaries, will not solve the NHS’s problems. Until then, await the next report and the inevitable political posturing.
This post was written by two old geezers who have been on the ground for over 30 years and shake their heads, awaiting the next political pantomime.








At least let's give credit to Mr Streeting for giving this veiled warning: "Streeting also said, "As a proportion of the NHS budget, we want to shift the balance in favour of neighbourhood services."
In real life this means 'increase community support for everything' - the old 'get rid of bed blockers by sending them to local community care homes'. Funny that there doesn't seem to be any mention of re-establishing and funding District nurses. After all, nurse practitioners are already a huge part of GP surgeries. This also means that local council taxes will need to rise, thus scrapping the single-person reduction in council tax will become a necessity: you all want to save the NHS, dontcha, so it's only fair to cough up. Perhaps it'll also get the 'ageing population (widows and widowers)' - ageing ever since baby boomers became the punchball for politicians trying to excuse their failings - out of their houses and into 'homes' where their clogs-popping can be accelerated.
And another thing: why 'digitalisation' is supposed to be the cure-all is beyond me. Do Messrs Streeting and Darzi not know how much installing and maintaining a properly working IT system costs? Or are they planning to let Big Pharma pay for it, in exchange for unlimited access to patient data?
Sorry, I'm just a bit peed off by this Darzi Report ...
Having run a veterinary hospital, I can come up with quite a few pointers:
1. Install good generalists at entrance of hospital, who can triage and refer to the relevant specialists if needed. Prevents people from ending up with the wrong specialist.
2. Work on personalised medicine rather than protocolised medicine.
3. Provide continuity of care, stop people from working in different hospitals.
4. Timely diagnostics, and subsequent reporting followed by prompt treatment.
5. Once diagnosed, treatment back to GP if possible.
6. Put healthcare back in the hands of health professionals.
7. You may want to consider that certain procedures are not essential and therefore not provoded by the NHS.
Just some ideas.
It is a behemoth, turning this ship around will be a Herculean task.